The paralysis tick presents more than just a backyard pest; a single bite can trigger a particularly bizarre condition in humans known as ‘mammalian meat allergy’.
Could this be your worst nightmare? Imagine the situation whereby your next bite of a pie, or chew on a steak could be the last, as eating red meat may well kill you. And so your days of carnivore delights and summer barbeques are suddenly over. But could this really happen? Well this is the fate of many people who are bitten by the Australian paralysis tick, Ixodes holocyclus, who suddenly develop a condition known as ‘mammalian meat allergy’. More on this later.
General information on Paralysis Ticks
In recent years the paralysis tick has become more common. Not only have its numbers grown dramatically, but the distribution of the tick has greatly spread. This means that more and more people are now being bitten by ticks and suffering the associated consequences of its bites. However, the growth in ticks also presents an opportunity for the savvy pest manager; increasingly, residents want control undertaken to ensure that their backyard is free of these biting pests. This article reviews the health impacts caused by ticks, why they are becoming a greater problem, and the various methods used for control.
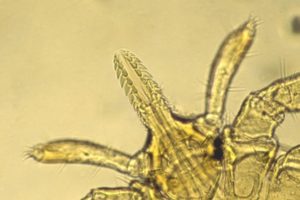
Ticks are blood-sucking parasites. There are around 75 different species in Australia and the most common that attacks humans is the Australian paralysis tick. The species occurs along the coastal strip of eastern Australia and is more abundant in native forests where native animals occur that serves as its main blood source and host. Ticks are more common in moist forests and are especially abundant on Sydney’s northern beaches and the hinterland of southeast Queensland. In these locations, encounters with humans are frequent.
Paralysis Tick Life-Cycle
Ticks have four distinct stages of development: egg, larva, nymph, and adult, which tends to be seasonal, although any stage may be encountered throughout the year. The larvae, nymphs, and adult females must have a blood meal from a host. After the blood meal, larvae and nymphs drop off the host and rest in the environment as they develop into the next stage. Adult females drop off the host and lay eggs in leaf litter. Ticks are not very mobile; larvae, nymphs and adults climb onto grass and the foliage of low bushes where they wait for passing hosts (animals or people) to feed on. Once on the host, ticks crawl upward on the host’s body to search for a place to attach, even onto the head. Despite the common belief, ticks do not drop out of trees.

Ticks abundance varies from season to season, but they are most numerous during wet years, which favours their survival. They are especially active after rain, particularly if there has been a continual spell of dry weather. Their numbers and distribution appear to be increasing in recent years due to successful fox control programs undertaken by councils. This has allowed the return of native animals, which provide a readily available blood source for ticks, swelling their numbers as well.
Tick Bites and Paralysis
While most tick bites produce only mild itching at the bite site, they can induce toxic effects such as paralysis, cause severe allergic reactions, and even transmit infectious diseases.
As the name implies, the paralysis tick can cause paralysis and in the past there were a number of human deaths. But with modern medicine and the availability of an anti-venene, there have been no deaths from paralysis since the 1940s. However, around 20,000 pets every year suffer tick-induced paralysis and sadly many succumb to the effects of the bite.
Regarding human health, allergic reactions are far more important, but also highly variable. Symptoms can range from itching at the bite site to a generalised allergic reaction (with rash and swelling), to even anaphylactic shock. A number of people have died in recent years from severe allergic reactions to tick bites.

Ticks Bites Can Cause Mammalian Meat Allergy
Without a question, one of the strangest consequences of a tick bite is the bizarre condition known as ‘mammalian meat allergy’ (MMA). During the bite, a chemical called ‘alpha gal’ can be passed on, which can later induce an allergic response following the consumption of mammalian meats. This includes beef, pork, lamb, kangaroo, and even whale and guinea pig, if travelling to such countries where these meats are served. Furthermore, patients with this condition must avoid all meat by-products such as gelatin. Meat products even appear in pineapple juice (used to clarify the juice) and in the lubricant on women’s sanitary products. Symptoms of MMA appear 2-10 hours after eating meat and may include abdominal pain, bloating and diarrhoea, welts, and even a life-threatening anaphylaxis. This condition is becoming more common with over 1,000 patients diagnosed with the condition just from the Sydney region alone.
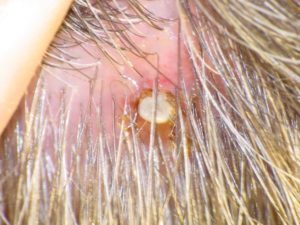
Typically, allergic reactions and paralysis become worse after the tick is removed. Attached ticks should not be touched, dabbed with chemicals or removed with tweezers. Rather they should be frozen in place with an ether-based spray that is used to treat warts and skin tags (e.g. Wartner, or Wart-off, both available from chemists) before removal. If the patient is known to suffer allergies from ticks, then removal should be undertaken in a safe setting, such as a doctor’s surgery or the emergency department of a hospital.
Other Tick Diseases
Finally, ticks can also transmit infectious diseases such as Queensland tick typhus (which is uncommon, yet treatable with antibiotics). Despite a lot of publicity in the gutter press, there is no evidence for Lyme disease in Australia.
Preventing Tick Bites
Avoiding tick-prone areas is a great way to prevent tick bites. Application of repellents to exposed skin, particularly with products containing DEET or picaridin, can reduce the risk of bites in tick-infested areas. Likewise, impregnating clothes with permethrin (available from outdoor stores) adds another layer of protection.
Tick Treatments
As humidity is important for tick survival, making the home environment drier will reduce tick numbers. This can be achieved by reducing overhanging foliage and allowing more sunlight to penetrate to the ground, keeping lawns mown, reducing leaf litter and the use of mulch, and minimising watering. Installing animal-proof fencing around the home will prevent animals from entering and the ticks they are carrying.
Insecticide applications are very effective at reducing tick numbers by more than 95% within a few hours. A range of pyrethroids are registered for use around the home including bifenthrin, beta-cyfluthrin, deltamethrin, esfenvalerate, and permethrin. A liquid formulation applied to the vegetation will kill ‘questing’ ticks (i.e. those waiting for a host), while a granular formulation will provide a good degree of ongoing control for 3-4 months.
For more information on ticks, the conditions they cause, and tick removal, see www.tiara.org.au (Tick Induced Allergies Research & Awareness).
Back to pest control ticks and more information on ticks.
Author and image credits, Stephen L. Doggett, Director, Department of Medical Entomology, Westmead Hospital, NSW


